
Below is a draft copy of the above article and is published here in accordance with the Authors promotional rights policy of Elsevier here. The below draft article is longer than the final accepted manuscript but has more detail
¬¬Title:
Prevalence, safety and effectiveness of ketamine for sedation of patients with acute behavioural disturbance during aeromedical retrieval: A retrospective chart review
Authors and affiliations:
Vinay GANGATHIMMAIAH, MBBS, MPH, FACEMa, Minh LE CONG, MBBS, FRACGP, FACCRM, FARGP, GDRGP, GCMAb, Mike WILSON, MBChB DIMC(RCSEd)a, Kate HOOPER, MBBSa, Andrew PERRY, MBBS, FACEM, PostGrad Cert Aeromedical Retrieval, Luke BURMAN, MBBS, BA(Mathematics & Sociology) FACEMa, Nathan PUCKERIDGE MParaSc(CritCare),BSc(ParaSc) c and Brian MAGUIRE DrPH, MSA, EMT-P c
aLifeFlight Retrieval Medicine, Townsville Base, PO Box 8300, Garbutt, Queensland 4814, Australia,
bRoyal Flying Doctor Service, Mount Isa Base,11 Barkly Highway, Mount Isa, Queensland, 4825, Australia
cSchool of Medical & Applied Sciences, CQUniversity Australia, Rockhampton Campus, Queensland, Australia.
Emails: vinay.gangathimmaiah@lifeflightmedical.org.au, mlecong@rfdsqld.com.au, searchandrescue@doctors.org.uk knhooper@gmail.org.au , andrew.perry@lifeflight.org.au , luke.burman@lifeflight.org.au , n.puckeridge@cqu.edu.au, b.maguire@cqu.edu.au
Corresponding author:
Vinay GANGATHIMMAIAH, MBBS, MPH, FACEM
Lifeflight Retrieval Medicine, Townsville Base, PO Box 8300, Garbutt, Qld 4814,Australia
E-mail: vinay.gangathimmaiah@lifeflightmedical.org.au
Phone: +61432650840
Abstract:
Introduc¬¬tion: The aim of this study was to determine the prevalence, safety and effectiveness of ketamine sedation in patients with acute behavioural disturbance(ABD) during aeromedical retrieval.
Methods: This was a retrospective observational study. Eligible patients were identified by searching the electronic databases of two aeromedical retrieval services in Queensland, Australia for adult patients with ABD who were transported between January 1st, 2015 and June 30th, 2016. Data abstraction was done as per standard chart review criteria. Incidence of intubations and incidence of adverse reactions were the main outcomes.
Results: 122 patients met inclusion criteria. 31(25.4%) patients were intubated, 21(17.2%) for airway protection/respiratory depression and 10(8.1%) for persistent ABD. 21(17.2%) patients received ketamine of whom 3(14.3%) were intubated for persistent ABD. 9(42.9%) patients developed hypertension post-ketamine of which 2 needed intervention. One patient developed hypoxia post-ketamine which resolved without intervention and one patient developed increased secretions. No patients developed nausea, vomiting, emergence phenomena, apnoea or laryngospasm.
Conclusion: Our study suggests that ketamine is a safe and effective agent for sedating patients with ABD during aeromedical retrieval.
Highlights:
17.2% of patients with ABD during aeromedical retrieval received ketamine sedation.
14.3% of patients who received ketamine sedation for ABD were intubated.
42.9% developed hypertension and 4.8% developed hypoxia post-ketamine sedation.
A small proportion of patients with adverse reactions needed intervention.
Introduction:
Acute behavioural disturbance(ABD), also known as Excited Delirium Syndrome, is a medical emergency with reported mortality of 8-10%.(1, 2) The management of ABD usually involves a judicious combination of de-escalation techniques, physical restraints and sedation.(1, 3, 4) Sedation of patients with ABD is usually accomplished with benzodiazepines and antipsychotics, either alone or in combination.(5, 6) The use of these two drug classes can be limited by several factors, primarily respiratory depression with benzodiazepines and a delayed onset of action of up to 20min with antipsychotics.(7, 8) In recent years, several small studies have explored the suitability of ketamine as an alternative agent for sedating patients with ABD in the prehospital, retrieval and emergency settings.(9-27) Favourable pharmacological properties including rapid onset of action of 2-5min, protection of airway reflexes and maintenance of respiratory drive make ketamine a promising sedative agent in the management of ABD.(28) Nevertheless, insufficient data about effectiveness and safety of ketamine in the setting of ABD have prevented it from gaining widespread acceptance for this indication.(29, 30) Firstly, the effectiveness of ketamine sedation in ABD, as measured by sedation failure rates, has varied between no failures in one retrospective study and 10% in a recent prospective study.(11, 19) Furthermore, the reported incidence of endotracheal intubations with ketamine has also varied widely between studies from 0-63%.(11, 17, 31, 32) Interestingly, a large study looking at the incidence of intubations in psychiatric retrievals before and after introduction of a ketamine sedation protocol for ABD found a decrease in incidence from 3.5% to 2.3%.(20) Finally, there is a lack of clarity about the minimum effective ketamine dose needed to achieve safe sedation of behaviourally disturbed patients with reported dose ranges of 0.5-1mg/kg as the initial intravenous dose followed by 1 – 5.56mg/kg/h intravenous infusion and 2.25- 9.42mg/kg as the total intramuscular dose. (11, 13, 23)
Along with benzodiazepines and antipsychotics, ketamine has been a part of the Standard Operating Procedure(SOP) for management of ABD at LifeFlight Retrieval Medicine(LRM), Queensland, Australia for over 3 years and Royal Flying Doctor Service(RFDS), Queensland, Australia for over 9 years. The objectives of this study were to determine the prevalence of ketamine use and to evaluate whether ketamine is a safe and effective alternative agent for sedation of patients with ABD in the aeromedical retrieval setting. The study hypothesis was that ketamine use results in a reduction in the incidence of endotracheal intubations in patients with ABD in the study setting compared to the reported incidence in existing literature. (20, 27, 31, 32)
Methods:
Design and Setting:
The study was a retrospective chart review of patients with ABD who were aeromedically retrieved by LRM and RFDS. LRM and RFDS are responsible for all aeromedical retrievals in Queensland, Australia and perform approximately 4700 and 11,500 retrievals per year respectively. Queensland is the second largest state in Australia with a land area of 1.73million square kilometres(33) and a population density of 2.7 people per square kilometre(34) resulting in prolonged, often challenging, retrievals of patients with ABD. LRM and RFDS employ a flight physician-flight nurse model for fixed-wing aircraft retrievals while LRM employs a flight physician-flight paramedic model for rotary-wing aircraft retrievals.
Ethics approval was granted by Central Queensland University Human Research Ethics Committee(H16/07-200).
Participant selection:
All patients with ABD needing aeromedical retrieval were included as study participants. ABD was defined as ‘any behaviour that puts the patient or others at immediate risk of serious harm and may include threatening or aggressive behaviour, extreme distress and serious self-harm which could cause injury or death’.(4) Patients were considered to have been sedated with ketamine if they received it exclusively for the management of ABD and not if they received it for analgesia, induction prior to intubation or sedation post-intubation. Patient records were identified by searching the electronic databases at LRM and RFDS between January 1,2015 and June 30,2016 using the following keywords: ketamine, droperidol, midazolam, diazepam, olanzapine, sedation, restraint, agitation, aggression, volatile, violence, behavioural disturbance, schizophrenia, psychosis, delirium, mania, psychiatric and mental health.
Outcome variables:
Incidence of intubations, incidence of adverse reactions, effective ketamine dose and duration of ketamine use were the outcomes of the study. We used the incidence of intubations as a surrogate measure of the effectiveness as we postulated that patients with ABD would have required intubation only if ketamine was ineffective in providing adequate sedation. Data was collected about patient demographics, route, dose and timing of sedatives, mode and duration of aeromedical retrieval, referring and receiving health facilities, presence of mental health order, use of physical restraints, co-morbidities, adverse reactions, any interventions to manage the adverse reactions and intubation timing and indication. Sedatives administered up to 12hours prior to the arrival of the retrieval team was considered as pre-retrieval sedation and all sedation after that point was considered as sedation during retrieval. Duration of retrieval was calculated from the time of arrival of the retrieval team at the patient to the time of patient handover to the receiving health facility including any road transfers between airport and the facilities. Data was collected about co-morbidities that could potentially alter the pharmacokinetics or pharmacodynamics of sedative agents. Adverse reactions were defined as follows: Hypertension-Systolic Blood Pressure(SBP) >140mmHg, Hypotension-SBP<90mmHg, Tachycardia-heart rate>100beats/min and Hypoxia-SpO2<90%. Data was also collected about other adverse reactions including nausea or vomiting, increased secretions, apnoea, laryngospasm and emergence phenomena. Intubations were considered as pre-retrieval if they were performed prior to boarding the aircraft including the ones performed by the retrieval team.
Data abstraction:
Data abstraction was done by study authors whilst adhering to standard chart review guidelines including abstractor training, explicit eligibility criteria, precise definition of variables, standardized abstraction forms, periodic meetings and performance monitoring. (35, 36) Interrater reliability was tested by a review of a sample of 20% of the charts. The abstractors could not be blinded to the study hypothesis as they were closely involved in design and conduct of the study. The data was abstracted from patient records after de-identification using a standardized data abstraction form and procedures manual. Data conflicts due to ambiguous, conflicting or erroneous data was resolved by periodic meetings and consensus between the abstractors.(37)Missing data was handled by case deletion.
Data analysis:
Data was analysed using SPSS (IBM SPSS Statistics for Macintosh, Version 24.0. Armonk, NY: IBM Corp). Continuous variables were tested for normality. Mean with Standard deviation and Median with Inter Quartile Range were calculated depending on distribution of the variables. Percentages with 95% confidence intervals were calculated for categorical variables. An online calculator was used to calculate the confidence intervals for proportions.(38) Interrater reliability was calculated using prevalence and bias adjusted kappa.(39)
Results:
122 out of 213 patients met inclusion criteria (Figure 1). Patient characteristics are shown in Table 1. 61.5% were male with a mean age of 35.8years. Fixed-wing retrievals accounted for 75.8% of all retrievals. Suicidal ideation or suicide attempt was the most common underlying aetiology for ABD accounting for 52.4% of all retrievals.
Sedation characteristics are shown in Table 2. 54.9% of patients received sedation pre-retrieval while 36.9% received sedation during retrieval. Diazepam and olanzapine were the two most commonly used sedatives pre-retrieval while midazolam and ketamine were the most common sedatives used during retrieval. Of the 122 patients, 31(25.4%) were intubated, 21(17.2%) for airway protection/respiratory depression and 10(8.1%) for persistent ABD. 21(17.2%) patients received ketamine during retrieval of which 3(14.3%) were intubated for persistent ABD.
Overall, 39(32.2%) patients had tachycardia, 32(26.4%) had an abnormal BP, and 10(8.3%) had hypoxia. Of the patients who received ketamine, 11(52.3%) developed tachycardia, 9(42.9%) developed hypertension, 1(4.8%) developed hypoxia and 1(4.8%) developed increased secretions. There were no reports of nausea, vomiting, emergence phenomena, apnoea or laryngospasm.
The doses and durations of ketamine use are shown in table 3. The median doses of ketamine for intubated and non-intubated patients were 1.2mg/kg/h (0.5-2.7) and 2.8mg/kg/h (1.6-3) respectively. The median duration of ketamine use was 120min (70-143).
There was moderate inter-rater agreement for abstraction of outcome data (observed agreement 85.2%, prevalence and bias adjusted kappa 0.70).
Discussion:
Key results
A significant proportion of our study participants did not need any form of sedation prior to or during aeromedical retrieval despite adverse environmental factors like vibration, noise and enclosed space that could precipitate or exacerbate ABD. This finding reinforces the importance of verbal de-escalation strategies in the management of ABD. Oral benzodiazepines and oral antipsychotics were the most commonly used pre-retrieval sedative agents in our study which is consistent with current practice. Parenteral sedative agents including ketamine were used infrequently during retrieval which is indicative of the significance of oral sedation in the management of ABD, particularly in the period leading up to patient retrieval. The finding that about a third of the patients were on an involuntary mental health order and in physical restraints during the retrieval is contrary to the experience of the study investigators and is likely an a result of underreporting.
We found an overall intubation rate of 25.1% for patients with ABD. Excluding patients who were intubated due to altered GCS from underlying etiology, we found an intubation rate of 8.1% for persistent ABD. This is higher than the rate of 2.3% reported by a 2015 study that looked at intubation rate in psychiatric patients who were aeromedically retrieved by RFDS, Queensland over a 10-year period. A closer look at the intubation rates in this study reveals a range of 0.95-4.7% with bases staffed by LRM physicians having higher rates of intubation than those staffed by RFDS doctors. The intubation rate in our study is consistent with the higher rate in the 2015 study as all intubations for persistent ABD were performed by LRM physicians.
The low incidence of failed sedation in our study indicates that ketamine is an effective sedative agent for ABD. We found an intubation rate of 14.3%(3/21) for patients receiving ketamine sedation in our study. This is lower than the reported intubation rates of 25%(32), 39%(17) and 63%(31) in three recent prehospital studies of ketamine sedation in ABD. There could be several explanations for this observed difference. Firstly, the three studies employed a fixed dose of intramuscular ketamine-unlike a titrable dose of intravenous ketamine in our study- which would have largely limited the ability to titrate sedation to effect. Secondly, ketamine was administered by critical care paramedics whose experience with ketamine sedation was significantly different to that of the retrieval physicians in our study. Finally, the three studies involved retrieval of patients with ABD with no prior sedation unlike our study which involved retrieval of patients with some form of prior sedation onboard(oral or parenteral or both) which could have reduced the required sedative dose of ketamine.
A detailed examination of the failed sedation cases revealed interesting findings. All three intubated patients were middle-aged males with known current stimulant drug use. All patients had received more than 500mg of intravenous ketamine and were receiving intravenous infusions at the rate of 1.6mg/kg/h, 2.8mg/kg/h and 3mg/kg/h at the time of decision to abandon sedation. There are two possible explanation for the failed sedations. One explanation is that these were cases of true sedation failure and the patients were ketamine non-responders. An alternative explanation is that the effective ketamine dose for these patients was probably higher and they could have been adequately sedated if the dose had been escalated further. This was borne out in one of the non-intubated patients in our study who needed a dose of 3.8mg/kg/h for adequate sedation. There have also been two unrelated case reports of successful ketamine sedation of similar patients with doses of 3.85mg/kg/h and 5.56mg/kg/h.(13, 21)
Our study results also indicate that ketamine is a safe sedative agent for acute behavioural disturbance. The incidence of adverse reactions in our study is similar to the reported incidence in literature except for nausea and vomiting(28, 40). One(4.8%) patient had transient hypoxia which resolved spontaneously. 9(42.9%) patients had hypertension of whom two(9.5%) needed a change in sedative agent to propofol due to a persistent SBP of 190mmHg. The absence of nausea and vomiting could be due to underreporting. It could also be due to the prevalent practice of routine administration of antiemetics (usually intravenous ondansetron) to all patients prior to fixed-wing aeromedical retrieval in Queensland. This effect has also been noted in paediatric studies where ondansetron was found to decrease the incidence of intravenous ketamine-associated vomiting (41, 42). The safety profile of ketamine remained unaffected by the duration of infusion with a maximum recorded duration of 170minutes.
We could not determine a median effective dose of ketamine for management of ABD due to a significant overlap in ketamine doses between patients with successful and failed sedation. It is possible that the effective dose of ketamine sedation is highly variable as evident from the dose range of 0.5-3.8mg/kg/h in our small study and is dependent on patient factors like recreational drug use that need further elucidation. It is also possible that there is a small proportion of patients with ABD who will not respond to ketamine regardless of the dose. Propofol might be a potential alternative agent for such patients, either alone or in combination with ketamine, as reported in one retrospective study.(27) These questions can be explored by future studies.
Limitations:
Our study has several limitations. The small sample size limits the strength of our conclusions. The absence of control group could have led to confounding. The electronic database search might have missed cases despite the comprehensive list of keywords thus resulting in selection bias. Deletion of cases with missing data might have resulted in measurement bias although it is unlikely to have altered the study conclusions. The incidence of adverse reactions and the ketamine dose might have been underestimated due to underreporting although this is unlikely due to consistency with reported incidence in literature. Finally, all patients in the ketamine sedation group also received prior sedation which could have biased the results overestimating the safety and effectiveness.
Conclusion:
Our study suggests that ketamine is a safe and effective alternative sedative agent for sedation of patients with acute behavioural disturbance during aeromedical retrieval. These findings can be further confirmed by adequately-powered prospective studies.
Contributions:
The study was designed by VG with advice from MLC, LB, MW, AP, KH, NP and BM. Data abstraction and analysis were performed by VG, MLC, MW, AP and KH. The final write-up was drafted by VG and was critically revised by MLC, LB, MW, AP, KH and BM.
Competing interests:
None declared.
Funding:
The study was unfunded.
References:
1. American College of Emergency Physicians White Paper on Excited Delirium Syndrome. 2009.
2. Vilke GM, DeBard ML, Chan TC, Ho JD, Dawes DM, Hall C, et al. Excited Delirium Syndrome (ExDS): defining based on a review of the literature. J Emerg Med. 2012;43(5):897-905.
3. The Royal College of Emergency Medicine Guidelines for the Management of Excite Delirium/Acute Behavioural Disturbance (ABD). 2016.
4. New South Wales Health. Management of patients with acute severe behavioural disturbance in the Emergency Departments
. 2015.
5. Kumar A, Datta SS, Wright SD, Furtado VA, Russell PS. Atypical antipsychotics for psychosis in adolescents. Cochrane Database Syst Rev. 2013(10):Cd009582.
6. Gillies D, Sampson S, Beck A, Rathbone J. Benzodiazepines for psychosis-induced aggression or agitation. Cochrane Database Syst Rev. 2013(4):Cd003079.
7. Thomas H, Jr., Schwartz E, Petrilli R. Droperidol versus haloperidol for chemical restraint of agitated and combative patients. Annals of Emergency Medicine. 1992;21(4):407-13.
8. Battaglia J, Moss S, Rush J, Kang J, Mendoza R, Leedom L, et al. Haloperidol, lorazepam, or both for psychotic agitation? A multicenter, prospective, double-blind, emergency department study. The American Journal of Emergency Medicine. 1997;15(4):335-40.
9. Burnett AM, Salzman JG, Griffith KR, Kroeger B, Frascone RJ. The emergency department experience with prehospital ketamine: a case series of 13 patients. Prehosp Emerg Care. 2012;16(4):553-9.
10. Burnett AM WB, Barringer KW, Griffith KR, Frascone RJ. Laryngospasm and hypoxia after intramuscular administration of ketamine to a patient in excited delirium. . Prehosp Emerg Care. 2012;16:412-4.
11. Le Cong M, Gynther B, Hunter E, Schuller P. Ketamine sedation for patients with acute agitation and psychiatric illness requiring aeromedical retrieval. Emerg Med J. 2012;29(4):335-7.
12. Ho JD, Smith SW, Nystrom PC, Dawes DM, Orozco BS, Cole JB, et al. Successful management of excited delirium syndrome with prehospital ketamine: two case examples. Prehosp Emerg Care. 2013;17(2):274-9.
13. Pritchard A, Le Cong M. Ketamine sedation during air medical retrieval of an agitated patient. Air Med J. 2014;33(2):76-7.
14. Scheppke KA, Braghiroli J, Shalaby M, Chait R. Prehospital Use of IM Ketamine for Sedation of Violent and Agitated Patients. Western Journal of Emergency Medicine. 2014;15(7):736-41.
15. Hopper AB, Vilke GM, Castillo EM, Campillo A, Davie T, Wilson MP. Ketamine use for acute agitation in the emergency department. J Emerg Med. 2015;48(6):712-9.
16. Keseg D, Cortez E, Rund D, Caterino J. The Use of Prehospital Ketamine for Control of Agitation in a Metropolitan Firefighter-based EMS System. Prehosp Emerg Care. 2015;19(1):110-5.
17. Cole JB, Moore JC, Nystrom PC, Orozco BS, Stellpflug SJ, Kornas RL, et al. A prospective study of ketamine versus haloperidol for severe prehospital agitation. Clin Toxicol (Phila). 2016:1-7.
18. Hayes BD. Ketamine for agitation: a key cog in the prehospital treatment armamentarium wheelhouse. Clin Toxicol (Phila). 2016:1-2.
19. Isbister GK, Calver LA, Downes MA, Page CB. Ketamine as Rescue Treatment for Difficult-to-Sedate Severe Acute Behavioral Disturbance in the Emergency Department. Ann Emerg Med. 2016;67(5):581-7 e1.
20. Cong ML, Humble I. A Ketamine Protocol and Intubation Rates for Psychiatric Air Medical Retrieval. Air Med J. 2015;34(6):357-9.
21. Reicher D. High-Dose Ketamine Sedation of an Agitated Patient During Air Medical Transport. Air Med J. 2016;35(2):84-5.
22. Kowalski. Ketamine for acute agitation adolescents. 2015.
23. Burnett AM, Peterson BK, Stellpflug SJ, Engebretsen KM, Glasrud KJ, Marks J, et al. The association between ketamine given for prehospital chemical restraint with intubation and hospital admission. Am J Emerg Med. 2014;33(1):76-9.
24. Hick JL, Ho JD. Ketamine chemical restraint to facilitate rescue of a combative “jumper”. Prehosp Emerg Care. 2005;9(1):85-9.
25. Melamed E OY, Ben-Avraham R, Blumenfeld A, Lin G. The combative multitrauma patient: a protocol for prehospital management. Eur J Emerg Med 2007;14(5):265-8.
26. Roberts JR GG. Intramuscular ketamine for the rapid tranquilization of the uncontrollable, violent, and dangerous adult patient. JTrauma. 2001;51(5):1008-10.
27. Soomaroo L, Mills JA, Ross MA. Air medical retrieval of acute psychiatric patients. Air Med J. 2014;33(6):304-8.
28. Green SM, Roback MG, Kennedy RM, Krauss B. Clinical practice guideline for emergency department ketamine dissociative sedation: 2011 update. Ann Emerg Med. 2011;57(5):449-61.
29. Schultz CH. Ketamine for pre-hospital control of agitated delirious patients: promising but not yet ready for prime time. The western journal of emergency medicine. 2014;15(7):742-3.
30. Green SM, Andolfatto G. Let’s “Take ‘Em Down” With a Ketamine Blow Dart. Ann Emerg Med. 2016;67(5):588-90.
31. Olives TD, Nystrom PC, Cole JB, Dodd KW, Ho JD. Intubation of Profoundly Agitated Patients Treated with Prehospital Ketamine. Prehospital and disaster medicine. 2016;31(6):593-602.
32. Hollis GJ, Keene TM, Ardlie RM, Caldicott DG, Stapleton SG. Prehospital ketamine use by paramedics in the Australian Capital Territory: A 12 month retrospective analysis. Emergency medicine Australasia : EMA. 2016.
33. Geoscience Australia[Internet]. Canberra,ACT. Geoscience Australia; 2016. Land areas of States and Territories ACT. [cited 2016 November 20] Available from: http://www.ga.gov.au/scientific-topics/national-location-information/dimensions/area-of-australia-states-and-territories.
34. Australian Bureau of Statistics[Internet]. Canberra,ACT. Australian Bureau of Statistics; 2016. Queensland state summary; 2016 March 29[cited 2016 November 20]. Available from: http://www.abs.gov.au/ausstats/abs@.nsf/Previousproducts/3218.0Main Features302013-14?opendocument&tabname=Summary&prodno=3218.0&issue=2013-14&num=&view=.
35. Gilbert EH, Lowenstein SR, Koziol-McLain J, Barta DC, Steiner J. Chart Reviews In Emergency Medicine Research: Where Are The Methods? Annals of Emergency Medicine. 1996;27(3):305-8.
36. Kaji AH, Schriger D, Green S. Looking through the retrospectoscope: reducing bias in emergency medicine chart review studies. Ann Emerg Med. 2014;64(3):292-8.
37. Gearing RE, Mian IA, Barber J, Ickowicz A. A Methodology for Conducting Retrospective Chart Review Research in Child and Adolescent Psychiatry. Journal of the Canadian Academy of Child and Adolescent Psychiatry. 2006;15(3):126-34.
38. Physiotherapy evidence database[Internet].Missenden,NSW. Centre of Evidence-Based Physiotherapy.2013. Herbert R. Confidence Interval Calculator; 2013 [cited 2016 December 28 ] Available from: https://www.pedro.org.au/english/downloads/confidence-interval-calculator/.
39. Byrt T, Bishop J, Carlin JB. Bias, prevalence and kappa. Journal of Clinical Epidemiology. 1993;46(5):423-9.
40. Deasy C, Babl FE. Intravenous vs intramuscular ketamine for pediatric procedural sedation by emergency medicine specialists: a review. Paediatric anaesthesia. 2010;20(9):787-96.
41. Langston WT, Wathen JE, Roback MG, Bajaj L. Effect of ondansetron on the incidence of vomiting associated with ketamine sedation in children: a double-blind, randomized, placebo-controlled trial. Ann Emerg Med. 2008;52(1):30-4.
42. Green SM, Roback MG, Krauss B, Brown L, McGlone RG, Agrawal D, et al. Predictors of emesis and recovery agitation with emergency department ketamine sedation: an individual-patient data meta-analysis of 8,282 children. Ann Emerg Med. 2009;54(2):171-80.e1-4.
FIGURES AND TABLES
Figure 1. Flowchart of participant recruitment
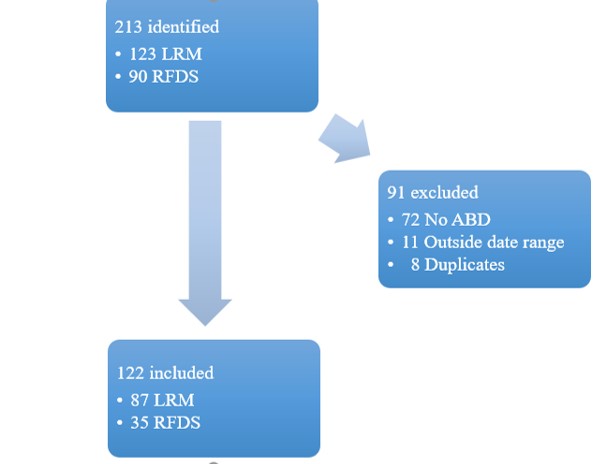
Table 1. Participant characteristics
Gender Male 61.5%( 75/122)
Female 38.5% (47/122)
Mean Age 35.8years (SD 16.3)
Retrieval mode Fixed-wing 75.8% (91/120)
Rotary-wing 21.7% (26/120)
Road 2.5% (3/120)
Comorbidities Present1 4.7% (6/122)
Absent 95.3% (116/122)
Diagnosis Suicide ideation / attempt 52.5% (64/122)
Schizophrenia 14.8% (18/122)
Psychosis NOS 9% (11/122)
Drug intoxication 9% (11/122)
Other2 14.8% (18/122)
Involuntary mental health order Present 34.4% (42/122)
Absent 63.6% (80/122)
Physical restraints Present 27% (33/122)
Absent 73% (89/122)
1Chronic respiratory disease(3), Chronic heart disease (3).
2ABD unknown cause(12), Smith-Magenis syndrome(2), Alcohol withdrawal syndrome(1), Trauma(1), Autism(1), Mania(1)
Table 2. Overall Sedation characteristics
Characteristics Incidence (Percentage; 95% Confidence Interval)
Sedatives Pre-retrieval1 None 67/122 (45.1%)
Diazepam 34/121 (28.1%)
Olanzapine 25/120 (20.8%)
Midazolam 16/121(13.2%)
Other2 28/121(23.1%)
During Retrieval None 77/122(63.1%)
Midazolam 26/122(21.3%)
Ketamine 21/122(17.2%)
Droperidol 12/122(9.8%)
Other3 21/122(17.3%)
Intubations4 Overall Airway/Respiratory issue 21/122(17.2%; 11.5-24.9)
ABD 10/122(8.2%; 4.5-14.4)
Ketamine Airway/Respiratory issue 0
ABD 3/21(14.3%; 5.0-34.6)
Adverse drug reactions5 Overall Abnormal BP 32/121(26.5%; 19.4-34.9)
Hypoxia 10/121 (8.3%; 4.6-14.6)
Ketamine Abnormal BP 9/21(42.9%; 24.5 –63.5)
Hypoxia 1/21(4.8%; 8.5-22.7)
Abbreviations:ABD Acute Behavioural Disturbance,BP Blood Pressure
1Upto 12hours prior to arrival of retrieval team.
2Haloperidol(12), Droperidol(10), Ketamine(3), Quetiapine(2), Risperidone(1).
3Diazepam(9), Olanzapine(6), Haloperidol(3), Propofol(2), Lorazepam(1).
4Incidence on intubations stratified based on ketamine use and indication for intubation.
5Incidence of adverse drug reactions stratified based on ketamine use and type of reaction.
Table 3. Ketamine sedation characteristics
Intubation status Mode1 of administration Dose of Ketamine Duration of infusion(minutes)
Bolus(mg) Infusion(mg/kg/h)
Intubated Infusion alone NA 2.8 120
Bolus +Infusion 530 1.6 70
Bolus + infusion 240 3.0 70
Not-intubated Infusion alone NA 0.5 35
Bolus + infusion 20 0.4 55
Bolus + infusion 50 0.5 120
Bolus + infusion 60 1.2 125
Bolus + infusion 60 2.5 143
Bolus + infusion 240 2.7 170
Bolus + infusion 60 3.8 165
Bolus + infusion 100 UTD2 120
Bolus alone 20 NA NA
Bolus alone 30 NA NA
Bolus alone 30 NA NA
Bolus alone 30 NA NA
Bolus alone 50 NA NA
Bolus alone 100 NA NA
Bolus alone 110 NA NA
Bolus alone 120 NA NA
Bolus alone 130 NA NA
Bolus alone 160 NA NA
Abbreviations: UTD Unable To Determine, NA Not Applicable
1 All doses administered intravenously
2Unable to determine due to missing weight;100mg given as infusion.

You must be logged in to post a comment.